Four years ago I blogged on how “The $1000 genome is a myth”. I think the first paragraph from that blog post is as relevant today as it was in 2015:
Barely a day goes by without a news story or social media post proclaiming that the $1000 genome now exists, and is ushering in a healthcare revolution. Every day, somebody, somewhere in the world, posts these graphs on Twitter. There’s even a Wikipedia page devoted to this topic. It’s a persistent news headline and, frustratingly, it’s currently wrong.
Since 2015, the health economic evidence base for genome sequencing has gradually expanded, and several cost estimates are now available, but overall I think we still lack the sort of rigorously conducted microcosting studies that can usefully inform resource allocation decisions regarding genomic testing.
Hopefully this paper that we published in Genetics in Medicine a couple of weeks’ ago can make such a contribution.
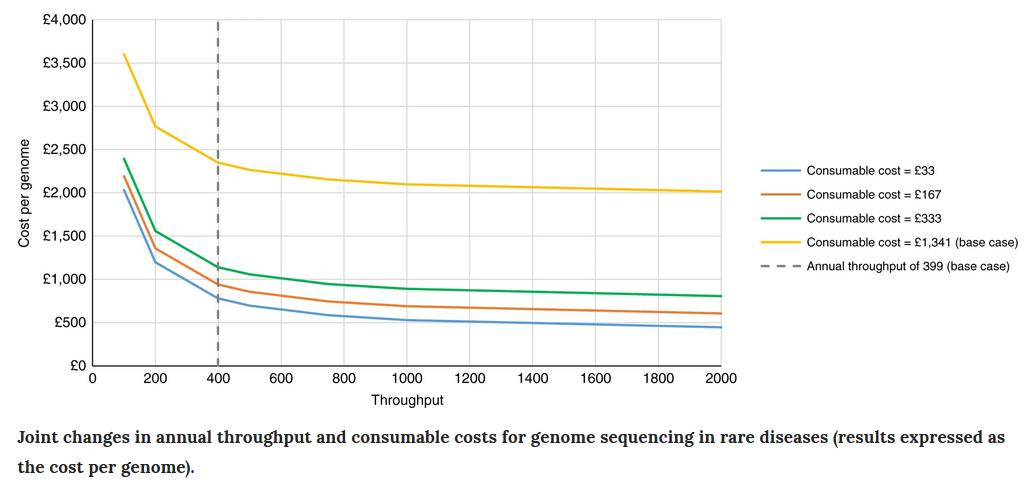
In this paper, we describe a microcosting study that we conducted of Illumina-based genome sequencing in cancer or rare diseases in a UK National Health Service laboratory processing 399 samples/year. We found that the costs of genome sequencing and clinical analysis of a cancer case or rare disease trio are substantially higher than this $1000 figure: £6841 (£3420 per genome) for cancer cases and £7050 (£2350 per genome) for rare disease cases. The consumables used during sequencing were the most expensive component of testing (68–72% of the total cost). We concluded that the costs of sequencing are yet to meet the desired $1000 per genome figure when testing is performed on relatively small numbers of patients with cancer or a rare disease in a single center with modest throughput. If we want to get to that desired $1000 per genome figure, the best route is likely to be combining high throughput — commensurate with a national-scale facility — with bulk discounts on consumable costs. The figure below illustrates this for sequencing of rare disease cases.
I’m pleased to see that there has already been a fair bit of interest in this paper online. I hope this will encourage researchers in other countries to generate similar cost estimates in their own country as this is just one study, and costs will almost certainly differ by setting and scale.